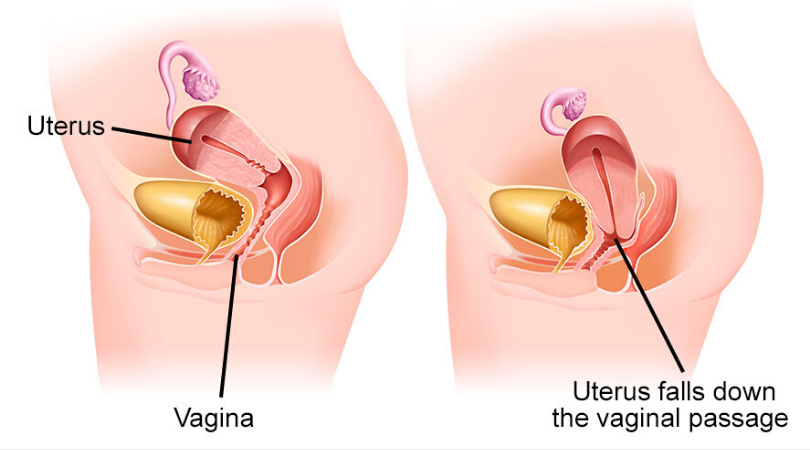
Uterine prolapse occurs when the uterus slips down from its normal position and protrudes into or outside the vaginal canal. This happens due to weakened pelvic floor muscles and ligaments, often as a result of childbirth, aging, or chronic pressure on the abdomen.
It is a common condition in postmenopausal women and those who have had multiple vaginal deliveries.
Causes of Uterine Prolapse
Several factors can contribute to the weakening of pelvic support structures, such as:
-
Vaginal childbirth, especially difficult or multiple deliveries
-
Aging and menopause (decreased estrogen weakens pelvic tissues)
-
Obesity or being overweight
-
Chronic constipation or straining during bowel movements
-
Chronic cough (due to smoking or lung conditions)
-
Heavy lifting over time
-
Pelvic surgery or injury
Symptoms
The severity of symptoms depends on the degree of prolapse. Common signs include:
-
A sensation of heaviness or pressure in the pelvis
-
Feeling of something "coming down" or bulging out of the vagina
-
Visible tissue protruding from the vaginal opening
-
Difficulty in urination or incomplete bladder emptying
-
Frequent urinary tract infections
-
Constipation or bowel movement problems
-
Lower back pain
-
Discomfort during sexual intercourse
In early stages, symptoms may be mild or even absent.
Stages of Uterine Prolapse
Uterine prolapse is classified into four stages, depending on how far the uterus has descended:
-
Stage 1 – Uterus drops slightly but remains inside the vagina
-
Stage 2 – Uterus descends close to the vaginal opening
-
Stage 3 – Uterus protrudes out of the vaginal opening
-
Stage 4 – Entire uterus is outside the vagina (also called complete prolapse)
Diagnosis
A gynecologist can usually diagnose uterine prolapse through:
-
Pelvic examination
-
Ultrasound (in some cases)
-
Urine tests to check for bladder involvement
-
Urodynamic testing (if urinary issues are present)
Treatment Options
Treatment depends on the severity of the prolapse, age, overall health, and whether the woman wishes to have children in the future.
Non-Surgical Treatment:
-
Pelvic floor exercises (Kegels) to strengthen muscles
-
Pessary device – a removable device inserted into the vagina to support the uterus
-
Lifestyle changes (weight loss, avoiding heavy lifting, treating constipation)
Surgical Treatment:
-
Uterine suspension – surgical repositioning of the uterus
-
Hysterectomy – surgical removal of the uterus (often recommended in severe or recurring cases)
-
Pelvic floor repair – tightening and reinforcing pelvic muscles and tissues
Prevention
-
Perform regular Kegel exercises to maintain pelvic strength
-
Maintain a healthy weight
-
Avoid chronic straining (treat constipation early)
-
Quit smoking to reduce chronic coughing
-
Avoid lifting heavy objects unnecessarily
-
Seek early treatment for urinary or bowel issues
Book Appointment


