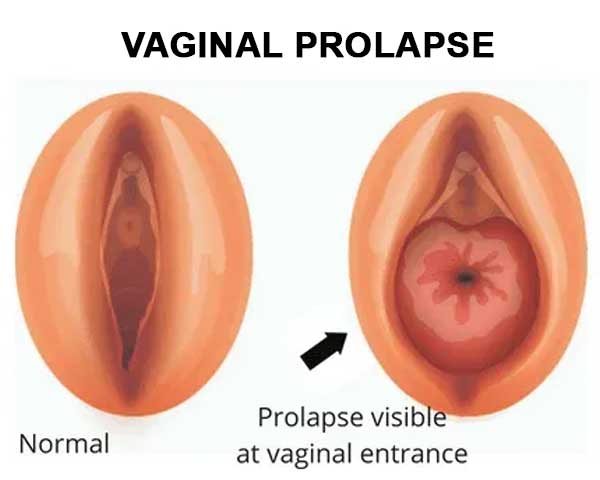
Vaginal Prolapse, also known as Pelvic Organ Prolapse, occurs when the vaginal walls or organs (like the bladder, uterus, or rectum) shift from their normal position and bulge into or outside the vaginal canal. This happens due to weakening of the pelvic floor muscles and ligaments, often as a result of childbirth, aging, or other health conditions.
It is a common condition, especially in women who have had multiple vaginal deliveries, are postmenopausal, or have undergone pelvic surgery.
Types of Vaginal Prolapse
Depending on the organ affected, vaginal prolapse may be categorized as:
-
Cystocele: Bladder bulging into the front vaginal wall
-
Rectocele: Rectum pushing into the back vaginal wall
-
Uterine prolapse: Uterus descending into the vaginal canal
-
Enterocele: Small bowel pressing against the upper vaginal wall
-
Vault prolapse: Vaginal top (vault) dropping down, especially after hysterectomy
Causes and Risk Factors
-
Vaginal childbirth (especially multiple or difficult deliveries)
-
Menopause and estrogen deficiency
-
Aging
-
Obesity
-
Chronic constipation or straining
-
Chronic coughing (due to asthma, smoking, etc.)
-
Heavy lifting or physically demanding work
-
Previous pelvic surgeries (like hysterectomy)
Symptoms of Vaginal Prolapse
-
Feeling of pressure, heaviness, or fullness in the vagina
-
Bulge or something “coming out” of the vagina
-
Difficulty in urinating or passing stools
-
Urinary leakage or urgency
-
Discomfort during intercourse
-
Lower back or pelvic pain
-
Symptoms worsen after prolonged standing or physical activity
Diagnosis
A gynecologist can diagnose vaginal prolapse through:
-
Physical and pelvic examination
-
Pelvic ultrasound (in some cases)
-
Urodynamic tests (if urinary problems are present)
Treatment Options
Treatment depends on the severity of the prolapse, age, general health, and future fertility plans.
1. Lifestyle Modifications
-
Weight loss if overweight
-
Avoiding heavy lifting and constipation
-
Pelvic floor exercises (Kegel exercises)
2. Vaginal Pessary
-
A removable device inserted into the vagina to support prolapsed organs
-
Useful for mild to moderate prolapse or for women who cannot undergo surgery
3. Surgical Treatment
Recommended for moderate to severe prolapse or when symptoms affect daily life:
-
Vaginal or laparoscopic repair of prolapsed tissues
-
Uterine suspension (to preserve the uterus)
-
Hysterectomy with pelvic floor repair (in some cases)
-
Mesh or native tissue repairs, depending on patient needs
Surgery is tailored based on the type of prolapse and patient preferences.
Recovery and Prognosis
Most women experience significant symptom relief after treatment. Regular follow-up, pelvic floor strengthening, and avoiding strain can prevent recurrence.
Book Appointment


